Story | Education
17 September 2020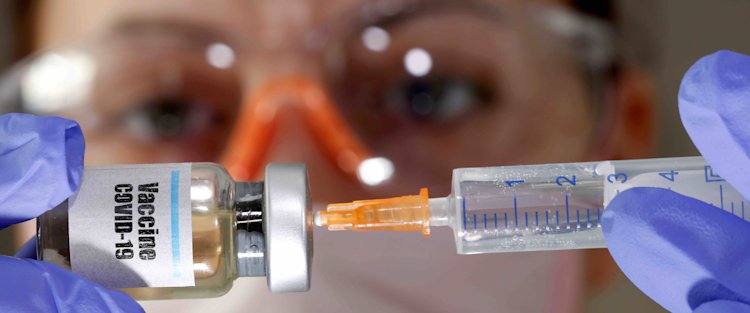
Medical specialists around the world are working on a COVID-19 vaccine.
Image source: Dado Ruvic, via REUTERSDr. Ali Sultan, Professor of Microbiology and Immunology at Weill Cornell Medicine-Qatar, explains how a vaccine is developed - and emphasizes the importance of scientific ethics being prioritized over individual national interests



